Everything You Should Know About Thrombosed Hemorrhoids and Hemorrhoid Treatment
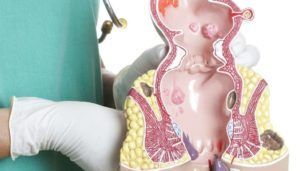
What is a thrombosed hemorrhoid?
Hemorrhoids are enlarged vascular tissue in your lower rectum and anus. That’s the opening at the end of your large intestine through which stool leaves your body. Everyone has hemorrhoids. They don’t cause problems unless they swell up, however. Swollen hemorrhoids can cause itching and pain around your anus that can make bowel movements uncomfortable. Fortunately, there are hemorrhoid treatments.
A thrombosed hernia is when a blood clot forms inside a hemorrhoid. This condition isn’t dangerous, but it can be painful.
Thrombosed hemorrhoid vs. regular hemorrhoid
There are two types of hemorrhoids:
- Internal hemorrhoids are inside your rectum.
- External hemorrhoids are around your anus.
What are the symptoms?
Thrombosed hemorrhoids can be very painful. If you have one, it can hurt to walk, sit, or go to the bathroom.
Other hemorrhoid symptoms include:
- itching around your anus
- bleeding when you have a bowel movement
- swelling or a lump around your anus
If you have a fever along with pain and swelling, you could have an area of infection called an abscess.
What causes thrombosed hemorrhoid?
You can get hemorrhoids from increased pressure on the veins in your rectum. Causes of this pressure include:
- straining while you have a bowel movement, especially if you’re constipated
- diarrhea
- irregular bowel movements
- pregnancy, from the force of the baby pressing on your veins or from pushing during delivery
- sitting for a long period of time, such as during a long car, train, or plane trip
What are the risks?
Hemorrhoids are very common. About three out of every four people will get at least one in their lifetime.
You’re more likely to get a hemorrhoid if you:
- are constipated because you don’t get enough fiber in your diet or due to a medical condition
- are pregnant
- often sit for long periods of times
- are older because aging can weaken the tissues that hold hemorrhoids in place
How is it diagnosed?
See your doctor or gastroenterologist near you if you have pain or itching around your anus, or if you bleed when you have a bowel movement. It’s important to see your doctor, because bleeding can also be a sign of cancer in the gastrointestinal (GI) tract.
Your doctor will ask about your symptoms and medical history. During the exam, they may insert a gloved, lubricated finger into your rectum to feel for any lumps or growths. This is called a digital rectal exam.
If you have signs or are at risk for colon cancer, you may need one of these exams to look deeper inside your colon.
- Sigmoidoscopy: The doctor inserts a thin, flexible scope with a camera at one end to view the bottom part of your colon. The scope allows your doctor to look for precancerous growths called polyps, and other changes in your colon.
- Colonoscopy : The doctor uses a scope to look at the entire length of your colon.
How is it treated?
Hemorrhoids are one of the conditions treated by a gastroenterologist. The main treatment for a thrombosed hemorrhoid is a procedure, called an external thrombectomy, that makes a small cut in the clot and drains it. You will get local anesthesia to prevent you from feeling pain.
This procedure works best if you have it within three days after the hemorrhoid appears. It works quickly, but the clots can come back. You might still have pain after surgery.
Treatment for regular hemorrhoids
You might be able to relieve the discomfort from hemorrhoids with a few simple home measures:
- Apply an over-the-counter hemorrhoid cream or ointment, such as Preparation H. You can also try a witch hazel wipe, such as Tucks.
- Take over-the-counter pain relievers like acetaminophen (Tylenol) and ibuprofen (Advil, Motrin IB)
- Sit in a warm bath for 10 to 15 minutes at a time, two to three times a day. You can use a sitz bath, which is a small plastic tub that immerses just your buttocks in a few inches of warm water. After your bath, gently pat, don’t rub, the area dry.
- Apply an ice pack or cold compress to the area.
Surgery for hemorrhoids
Less than 10 percent of people with hemorrhoids will need surgery. You may need surgery if your hemorrhoid is very large or if you have both external and internal hemorrhoids.
Types of surgery for hemorrhoids include:
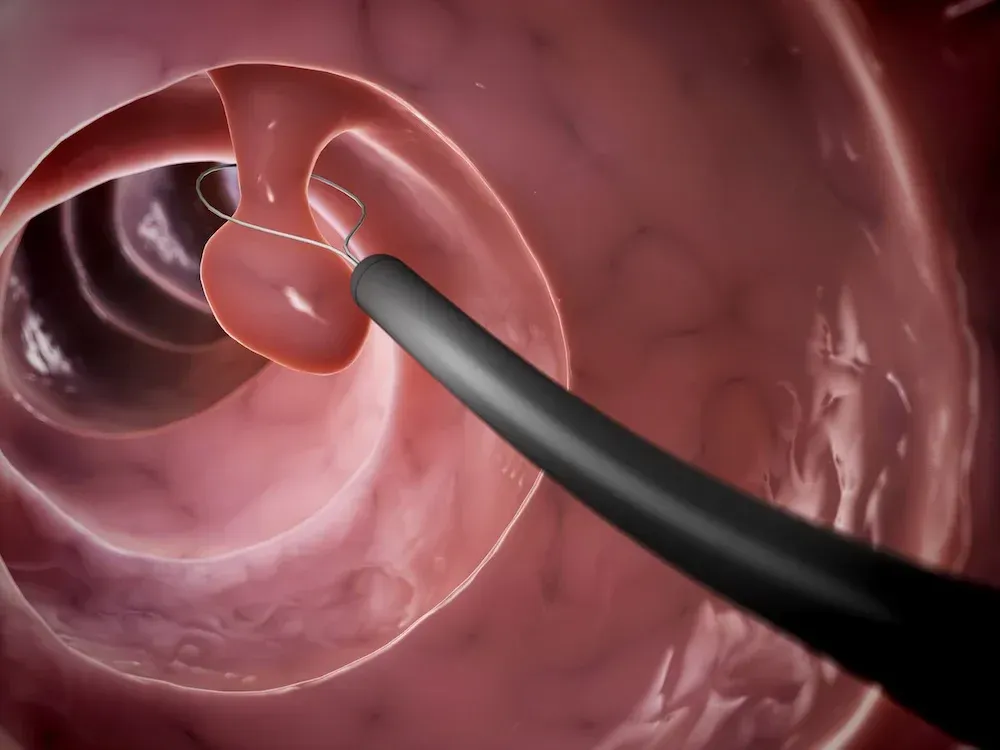
Rubber band ligation: The doctor places a small elastic band at the base of the hemorrhoid. In a few weeks, the hemorrhoid should shrink.
Hemorrhoidectomy: This procedure removes the hemorrhoid, along with the clot and blood vessels. You may get a spinal block, which numbs the area of surgery, or you might be asleep under general anesthesia during this procedure. This procedure is more invasive and takes longer to perform than an external thrombectomy, but the hemorrhoid is less likely to come back. It’s usually only done for the most severe hemorrhoids because it causes much more pain. Side effects of this surgery include pain, urinary tract infections, and trouble emptying your bladder.
Stapled hemorrhoidopexy: This procedure is also done while you’re asleep under general anesthesia. The surgeon uses a stapling instrument to put the hemorrhoids back in place and hold them there.
How long does recovery take?
The pain of thrombosed hemorrhoids should improve within 7 to 10 days without surgery. Regular hemorrhoids should shrink within a week. It may take a couple of weeks for the lump to completely go down.
You should be able to resume most activities right away. While you’re healing, avoid intense exercise and other strenuous activities.
Hemorrhoids can come back. Having hemorrhoidectomy surgery reduces the likelihood that they’ll return.
What are the complications?
Thrombosed hemorrhoids don’t usually cause complications. They can be very painful and they might bleed, however.
What is the outlook?
Sometimes your body will absorb the clot from a thrombosed hemorrhoid, and the hemorrhoid will improve on its own within a week or two. If you have surgery within three days of when the thrombosed hemorrhoid appears, it can relieve pain and other symptoms.
How are hemorrhoids prevented?
To avoid hemorrhoids in the future:
- Get more fiber in your diet from fruits, vegetables, and whole grains like bran. Fiber softens stool and makes it easier to pass. Try to get around 25 to 30 grams of fiber a day. You can take a fiber supplement such as Metamucil or Citrucel if you don’t get enough from diet alone.
- Drink about eight glasses of water daily. This will prevent constipation and the straining that causes hemorrhoids.
- Exercise regularly. Keeping your body moving will keep your bowels moving too.
- Set aside time each day to go. Staying regular can help prevent constipation and hemorrhoids. If you have to make a bowel movement, don’t hold it in. Stool can start to back up, forcing you to strain when you go.
Read More About Hemorrhoids Diagnosis and treatment
External Hemorrhoids Information Guide
Hemorrhoids Diagnosis and treatment
Symptoms of hemorrhoids that you must identify
The post Everything You Should Know About Thrombosed Hemorrhoids and Hemorrhoid Treatment appeared first on Gastro SB.