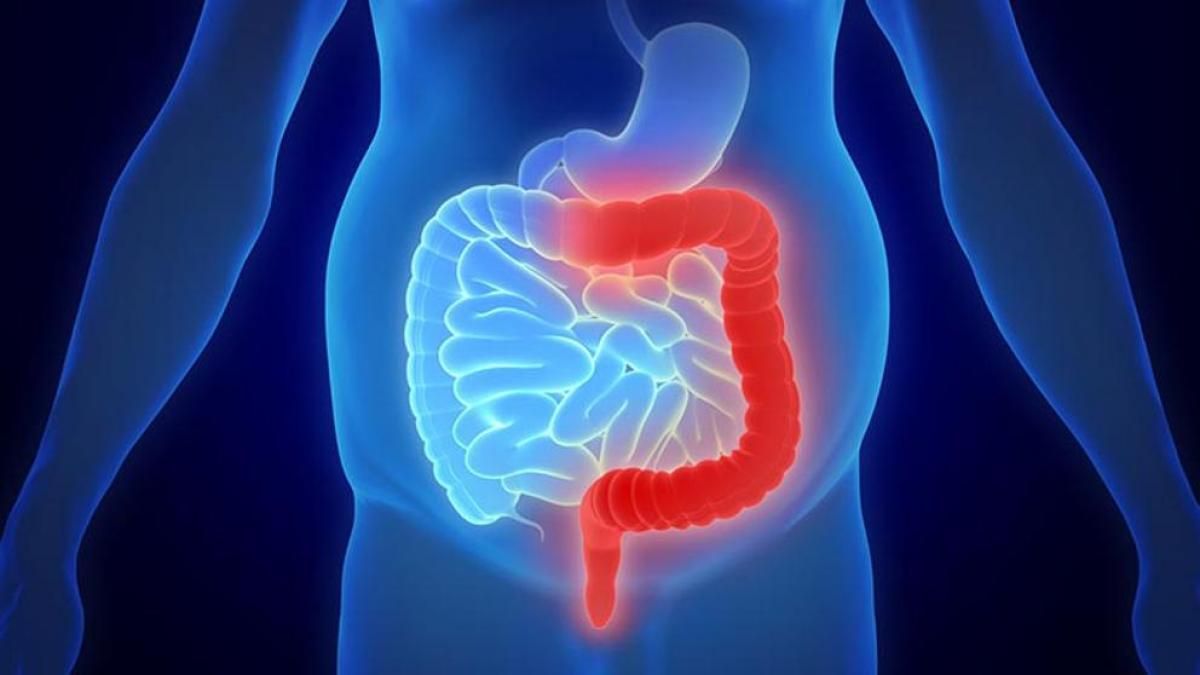
Patient Education: Blood in the Stool (Rectal Bleeding) in Adults (Beyond the Basics)
INTRODUCTION It can be scary to see blood in the toilet or when you wipe after a bowel movement. Fortunately, most of the causes of rectal bleeding are not life-threatening; common causes include hemorrhoids and anal fissures, which are discussed below. However, the only way to be certain of the cause is to be evaluated by a health care provider, such as a gastoenterologist.This article will discuss when to seek help for rectal bleeding, the most common causes of blood in the stool, and tests that may be recommended.
WHEN TO SEEK HELP Most people with minor rectal bleeding do not have colon cancer or another serious condition. However, it is not possible to know the cause of bleeding without an examination by a clinician. For this reason, if you ever notice blood in your stool or bleeding from your rectum, you should contact your health care provider as soon as possible. They can give you advice about whether and when you should be examined or schedule tests.
You should also seek medical care if you notice a change in the frequency or consistency of your bowel movements, have abdominal pain, or feel very tired or weak.
RECTAL BLEEDING CAUSES
Common benign (non-serious) causes — If you see a small amount of bright red blood on the toilet paper after wiping, on the outside of your stool, or in the toilet, this may be caused by hemorrhoids or an anal fissure. Both of these conditions are benign, and there are hemorrhoid treatments and medications that can help.
Hemorrhoids — Hemorrhoids are swollen blood vessels in the rectum or anus that can be painful, itchy, and sometimes bleed. People with hemorrhoids often have painless rectal bleeding; bright red blood may coat the stool after a bowel movement, drip into the toilet, or stain toilet paper. More information about hemorrhoids is available separately.
Hemorrhoids
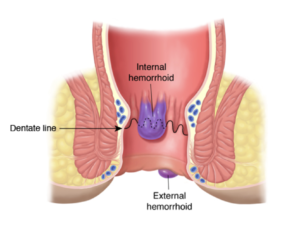
The dentate line divides the anal canal into two parts. Internal hemorrhoids originate from above the dentate line; external hemorrhoids originate from below the dentate line.
Anal fissure — An anal fissure is a tear in the lining of the anus (the opening where stool exits the body). Anal fissures can cause bleeding and a sensation of tearing, ripping, or burning pain during or after a bowel movement. This is discussed more separately.
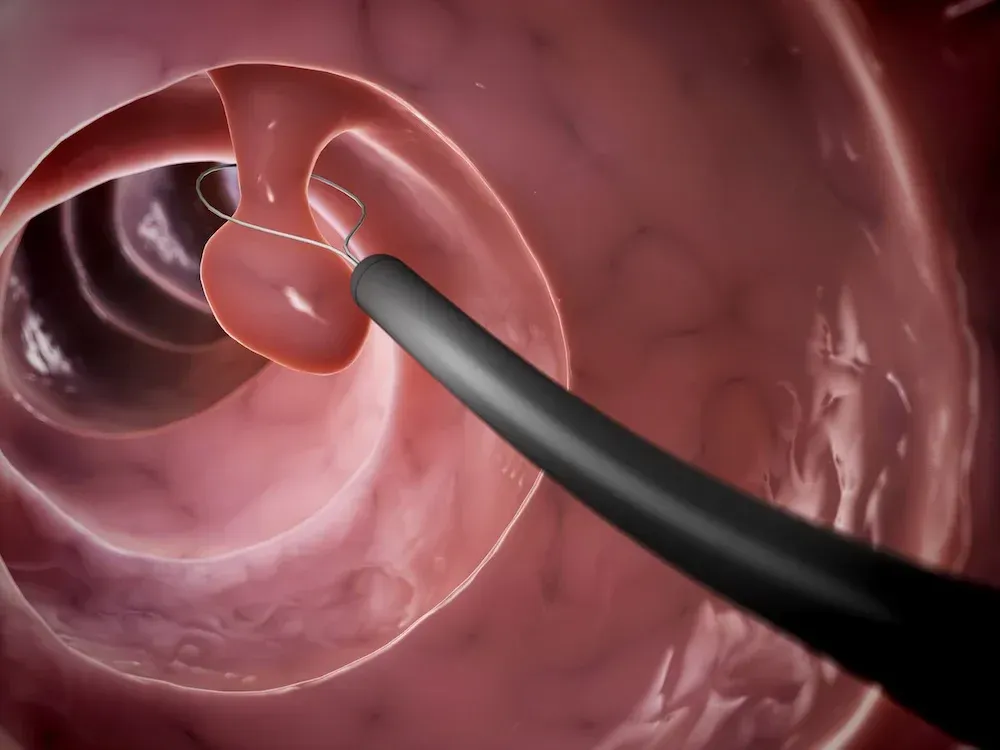
Serious causes — While most rectal bleeding is caused by the non-serious causes mentioned above, it can also be caused by cancerous or precancerous conditions. Precancerous polyps near the end of the colon (large intestine) can mimic bleeding from hemorrhoids. These polyps are generally present in the colon for years before they become cancerous, and they can be removed very safely from the colon, preventing progression to cancer.
Colorectal cancer is sometimes diagnosed in people who have ignored bleeding for years because they assumed it was from hemorrhoids. This is why anyone with rectal bleeding should consult a health care provider to determine the cause. If colorectal cancer is diagnosed early, it can often be treated.
The risk of polyps and colon cancer increases with age; this is why screening tests are usually recommended beginning at age 45 to 50 years, or earlier for people with certain additional risk factors.
Other possible causes — There are other causes of rectal bleeding as well, including colitis (inflammation of the colon), proctitis (inflammation of the rectum), diverticular disease, angioectasias (abnormal blood vessels in the gastrointestinal tract), and rectal ulcers.
Bleeding from higher in the digestive tract, such as the stomach, can cause black, tarry-looking bowel movements; this is because stomach acid turns blood black. In other cases, however, upper gastrointestinal bleeding appears bright red in color.
Your health care provider can figure out the cause of your bleeding based on your symptoms and test results.
RECTAL BLEEDING TESTS
The best approach to determining the cause of rectal bleeding depends upon your age, symptoms, and medical history. Your health care provider can learn more by asking questions about your bleeding (including frequency, amount, and appearance), bowel habits, whether you have other symptoms such as pain, and your family history (for example, if you have relatives who have been diagnosed with colorectal cancer or other cancers).
Physical examination — Sometimes a health care provider can determine the cause of rectal bleeding with a rectal examination. This typically involves inspecting the outside of the anus and inserting a gloved finger into the rectum to feel for lumps or other abnormalities. An anoscopy may be done at the same time. During an anoscopy, the clinician uses a rigid tube to inspect the anal canal and lower rectum. This can be done in the office and does not require sedation.
Diagnostic tests — There are several tests that allow a provider to examine the inside of the colon, rectum, and anus. These procedures are performed using specialized instruments called “scopes”:
- Sigmoidoscopy — During a sigmoidoscopy, a clinician can examine the rectum and most of the lower large intestine.
- Colonoscopy — A colonoscopy is a procedure in which a clinician examines the entire colon.
While the recommended tests may be different for different people, the important thing is to see a health care provider for evaluation. This is the only way to figure out for sure what is causing your rectal bleeding and get you the care and treatment you need.
Source : Uptodate®
The post Patient Education: Blood in the Stool (Rectal Bleeding) in Adults (Beyond the Basics) appeared first on Gastro SB.